Last month’s edition of Making
Good Healthcare Better focused upon Business Process Management and
identified five key components of it.
The first is identifying critical processes, the focus of this
newsletter.
Why is it necessary to actively manage key or critical
processes? In order to thrive in a
changing reimbursement and regulatory environment key processes need to be
optimized and new ones implemented. In a
recent speech, the CEO of Metro Health, Mike Faas, located in Wyoming,
Michigan, stated that in order to succeed his organization needed to form new
partnerships with regional providers. He
stated that one goal was to keep patients out of the hospital and to treat them
more effectively by primary care physicians.
Patient panels for physicians would need to almost double in size from
the current average of 2000. The best
way to do this was to improve processes at the primary care site with teamwork
and to establish better communications with partners. I believe that this strategy will be
necessary for most hospital groups.
The passage of the Medicare Access and Chips Reauthorization
Act (MACRA) focuses on improved outcomes for patients and new payment options
for physicians. Eligible providers must
choose one of two options in order not to have their reimbursements cut. One way to do this is through quality
reporting: Merit-Based Payment Systems
(MIPS). MIPS will be based upon four
measures—quality, efficiency, meaningful use of EHR’s and clinical practice
improvement activities; all are process based.
The makeup of MIPS will be determined by May 1, 2016. More than likely PQRS and VBPM, two current
reporting processes, will be integral to MIPS.
MIPS will require that eligible physicians and their groups focus more
on teamwork and manage and improve key processes.
If management and improvement of key processes will increase
in importance soon (the best providers and businesses are already involved in
this) it will be necessary for us to understand what processes are and
understand how to identify key processes.
I believe that the American Society of Quality has some of
the best resources available for understanding and improving processes (I am a
member). As found in last month’s
newsletter, they define Process as “A
set of interrelated work activities characterized by a set of specific inputs
and value added tasks that make up a procedure for a set of specific outputs.” One of the best ways to see processes is to
organize the activities of the process into a flow chart or, as used in Lean
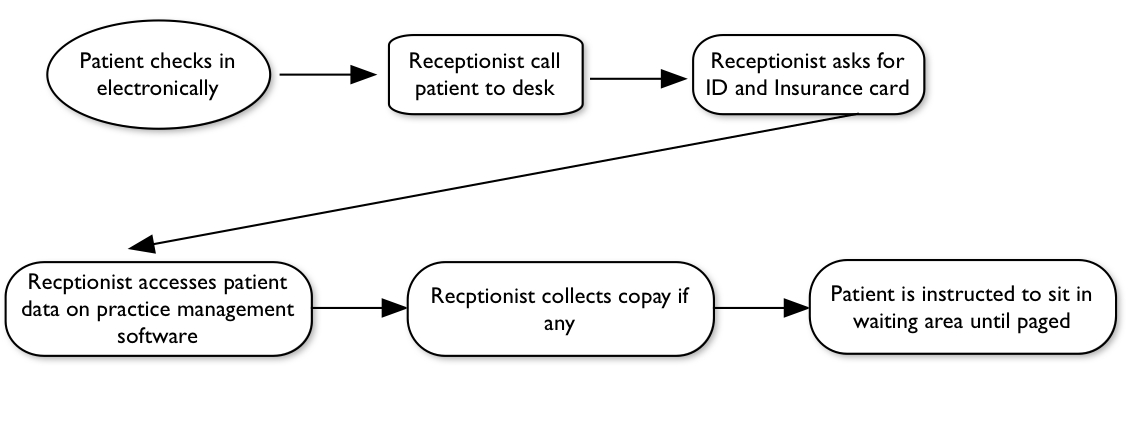
Healthcare, a value stream map. Below
you will find a very simple flow chart of checking in a patient at an
outpatient clinic. Not every activity is
included in this flow chart, only the key ones.
It is not necessary to state every activity in a flow chart. The level of detail in a flow chart is
determined by its use. The following one
details the key interactions between the receptionist and patient. Other steps that could be included would be
the notification to providers that the patient has checked in and is ready to
be seen. Thus, the check-in process:
There are many
processes, many interrelated, at a site, whether it is a provider,
manufacturing, or business site. It is
not possible to identify all of them in most circumstances. For the success of a business it is necessary
to manage and improve the critical ones.
After these are managed and continuous improvement implemented, less
important processes can be focused upon.
How does one identify key processes? I believe that one should use the following
steps, which I will explain in more detail afterwards:
- Form a leadership team to identify the key processes
- Identify criteria that can be used to gauge importance of a process
- Leadership seeks to understand basic steps of processes being examined
- Decide which processes are critical and sort them by order of imporatnce
1.
Decisions about critical processes need to be decided by the
leaders and executives of a provider or business. In order to manage and improve processes
leadership must be engaged and be supportive.
Also, leadership is likely the only group aware of all the important
processes at a site. Thus, they must be
initially involved in setting priorities.
In order to rank and prioritize processes some agreed upon
criteria must be defined. One criterion
might be the cost of the failure to manage the process. For example, if physicians and clinical staff
do not keep up with their certification process, an outpatient clinic could
fail. If a food manufacturer does not
insure the safety of its food by inspection it may be heavily fined. Another criteria besides monetary costs could
be the meeting of regulations. For
example, if banks fail to have adequate reserves they can be fined by the
Federal Reserve.
It is necessary for each leader on the decision team to
understand the basic steps of the processes under consideration. If they do not, it will be difficult to
prioritize the processes. If a leader(s)
do not know the basic steps he should go-and-see the process in action.
Lastly, all the processes under consideration should be
ranked by the leadership team in order of importance based upon the criteria
decided upon by the team. The first ones
should be focused upon. A timeline for
improving the management of the process should be set and a champion from the
team identified to oversee its improvement and management.
As you can see, identifying key process at a site is very important
to the health of any business. Failure
to do so will lead to the loss of potential revenue and negatively impact
customers and patients. Identifying the
key processes takes time and effort by leadership but is well worth the
investment. The steps identified will
lead to an effective identification and prioritization of key and critical
processes.
#PatientCareSystems #QualityManagement #processmanagement #PatientFlow